Strategies to improve adherence involve identifying and addressing potential barriers. The health professional’s approach influences how comfortable a patient is in providing a true report of adherence. Good interviewing techniques include a caring, non-judgemental approach and allowing enough time to discuss these issues. There are many ways to address barriers to adherence such as polypharmacy, physical impairment, side-effects, poor understanding and cost.
Complex regimen and frequent changes in treatment
- Simplify medication regimen by minimising the number of medicines or the frequency of administration (such as using longer-acting formulations) where possible
- Encourage use of dose administration aids (see images below) such as a Dosette Box (patient or Pharmacy packed) or Webster Pak® (Pharmacy packed)
- A range of smart phone medication reminder application are available
- Advise the patient to attend the same pharmacy for all of their prescriptions
- Encourage the patient to seek advice from the pharmacist, medical officer or nurse before taking any OTC medications or herbal and vitamin supplements
- During the period of titration of medicines, patients should be advised why and when dose adjustments will be made. Ideally, provide a current medication list or medicines plan with each change in therapy
- Encourage patients to keep a current medication list with them at all times
- Minimise changing brands, to avoid patient confusion
Figure 1: Dose administration aids for patients
Weekly Dosette box
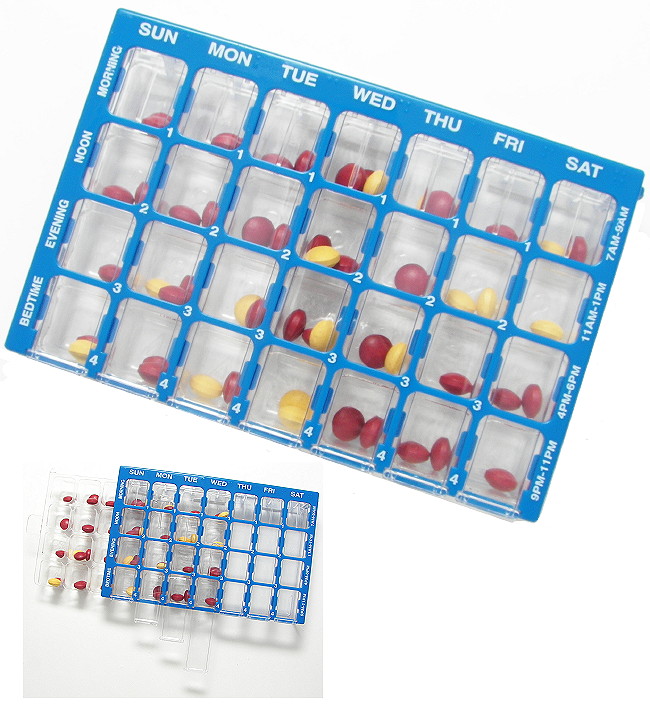
Reproduced with permission from www.forgettingthepill.com
Webster Pak®
010615b.jpg)
Image courtesy of Webstercare. Webster-pak® is a registered trade mark of Manrex Pty Ltd
Physical impairments
Consider the appropriateness of dose formulation for administration (such as for swallowing difficulties)
Provide instructions in large print
Enlist the aid of a carer or family member in administering medications
Consider aids to open containers (e.g., medications blister pack opener, medical bottle openers, tablet cutters) when appropriate
Side effects
Common side effects from medicines used in secondary prevention of CAD include bleeding, bruising, dizziness, cough and muscle ache. Side effects from HF medications may include inconvenience of diuresis, fatigue and dizziness from beta-blockers, or dizziness and cough from ACEIs.
Diuretics can be administered in the morning and afternoon to minimise nocturia. Patients should not skip doses but may adjust the timing to avoid inconvenience when access to a toilet is limited.
Discuss the risk versus benefit of each medicine with the patient. Work in partnership with each patient to identify and manage potential side effects and to determine when a medical review is required.
Poor understanding
Poor understanding of the benefits of medications, for example, during the initiation and up-titration of beta-blocker therapy, may contribute to poor adherence as patients may experience symptoms such as dizziness and fatigue before noticing the benefits of therapy.
- Patient education should include the explaining the purpose of each medicine, how to take it, and its therapeutic effects, precautions and adverse effects. See suggested outline for group medications education sessions
- Regularly reinforce the benefits of therapies, and discuss the importance of continuing to follow recommended treatment dosing schedules
- Promote shared decision-making by provide patients with an opportunity to express their concerns about medicines and address these if possible
Cost
During dose up-titration of a medicine, multiple prescriptions for different strengths of the medicine may be required, which some patients may find a financial burden. Ensure patients are aware of any available government subsidies and advise them to discuss dose changes with their doctor before they decide to stop taking any medication. More cost-effective generic equivalents may be prescribed in cases where changes to a branded medicine will not cause any detrimental effects to the patient in terms of efficacy or safety or patient acceptance.
For more information see the National Heart Foundation of Australia Improving adherence in cardiovascular care toolkit.[#national-heart-foundation-of-australia-aslani-p-krass-i-bajorek-b-thistleth]
 Pathophysiology
Pathophysiology
 Treatment & Management
Treatment & Management
 Exercise
Exercise
 Medications
Medications
 Psychosocial Issues
Psychosocial Issues
 Patient Education
Patient Education
 Behaviour Change
Behaviour Change
 Clinical Indicators
Clinical Indicators
 Pathophysiology
Pathophysiology
 Treatment & Management
Treatment & Management
 Exercise
Exercise
 Medications
Medications
 Psychosocial Issues
Psychosocial Issues
 Patient Education
Patient Education
 Behaviour Change
Behaviour Change
 Clinical Indicators
Clinical Indicators
 Pathophysiology
Pathophysiology
 Treatment & Management
Treatment & Management
 Exercise
Exercise
 Medications
Medications
 Psychosocial Issues
Psychosocial Issues
 Patient Education
Patient Education
 Behaviour Change
Behaviour Change
 Clinical Indicators
Clinical Indicators



010615b.jpg)